New study finds a potential new treatment approach to stopping a kind of childhood brain tumor from spreading onto the spine, as released today in the journal Scientific Reports www.nature.com/articles/srep27012 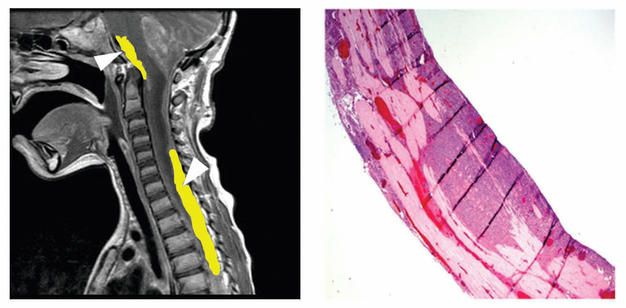 [ Figure Legend: (left) white arrowheads point to tumor cells in yellow covering the brain stem and spine. (right) on the spine, pink, are seen a thick covering of tumor cells, blue.] [press release] Portland, OR, June 3, 2016 – Researchers at the Children’s Cancer Therapy Development Institute (cc-tdi.org) have uncovered a protein that explains how brain tumor cells are attracted to new sites in the brain and along the spine. The childhood brain tumor is called medulloblastoma. It is the most common brain tumor of childhood. Medulloblastoma has a problematic tendency to spread (metastasize). This tendency to spread is so great that radiation to the brain and spine are standard treatments. However, radiation has its cost – causing permanent damage to both the child’s growth and learning abilities. For this reason, radiation is delayed as long as possible to give the child’s brain time to mature. But a substitute for radiation is elusive until now. Lead author and cc-TDI scientist Matthew Svalina explains, “we discovered that 2-way communication was happening between the normal covering of the spine and tumor cells – inadvertently making the covering a rich soil for tumor seeding.” The communication occurs through a growth factor called IGF1, which can be blocked by inhibiting its receptor. The authors also show that a clinically-investigated drug developed for adult colon cancer that blocks the receptor for IGF1 in childhood medulloblastoma can impair survival of tumor cells. According to cc-TDI scientific director Dr. Charles Keller, “Now that we understand this important mechanism of tumor spreading, we can repurpose shelved drugs from pharmaceutical companies as potential treatments for these children. There will be more testing involved before a clinical trial is proposed, but we think we’re on the right track. Preventing the side effects of radiation while curing the tumor is our highest priority.”
[ Figure Legend: (left) white arrowheads point to tumor cells in yellow covering the brain stem and spine. (right) on the spine, pink, are seen a thick covering of tumor cells, blue.] [press release] Portland, OR, June 3, 2016 – Researchers at the Children’s Cancer Therapy Development Institute (cc-tdi.org) have uncovered a protein that explains how brain tumor cells are attracted to new sites in the brain and along the spine. The childhood brain tumor is called medulloblastoma. It is the most common brain tumor of childhood. Medulloblastoma has a problematic tendency to spread (metastasize). This tendency to spread is so great that radiation to the brain and spine are standard treatments. However, radiation has its cost – causing permanent damage to both the child’s growth and learning abilities. For this reason, radiation is delayed as long as possible to give the child’s brain time to mature. But a substitute for radiation is elusive until now. Lead author and cc-TDI scientist Matthew Svalina explains, “we discovered that 2-way communication was happening between the normal covering of the spine and tumor cells – inadvertently making the covering a rich soil for tumor seeding.” The communication occurs through a growth factor called IGF1, which can be blocked by inhibiting its receptor. The authors also show that a clinically-investigated drug developed for adult colon cancer that blocks the receptor for IGF1 in childhood medulloblastoma can impair survival of tumor cells. According to cc-TDI scientific director Dr. Charles Keller, “Now that we understand this important mechanism of tumor spreading, we can repurpose shelved drugs from pharmaceutical companies as potential treatments for these children. There will be more testing involved before a clinical trial is proposed, but we think we’re on the right track. Preventing the side effects of radiation while curing the tumor is our highest priority.”  [ Keith, age 4 ] Darcee and Brent Burnett’s son, Keith, was a child affected by medulloblastoma. Darcee comments, “Our experience with metastatic medulloblastoma was devastating. We literally watched our son, Keith deteriorate before our eyes. The treatment options were grim considering we had no guarantee they would work and even if they did, there were serious lifelong side-effects. Once the initial treatment didn’t work, we had no options. There was no plan available for treatment. That is something no parent should ever hear.It was important to us that after he passed, Keith’s tumor tissue was donated to research in hopes of finding better treatment options. We miss him more than can be imagined and in his memory, it is our goal to continue to fund research like this to help other children and families from heartache and loss. We are grateful and extremely hopeful by these research findings.” Anne and Kent White had a similar experience for their affected son, Zach. “My son Zach was diagnosed with medulloblastoma at the age of 4. He endured fifteen months of surgery, chemotherapy and radiation, yet the cancer returned. At that time, there was no hope of survival. The doctors did not have any proven treatments to deal with Zach’s cancer once it metastasized. As a parent it is devastating to look at your beautiful, vibrant child and know their fate is sealed because of a 3 mm. spot on their brain. As a parent your instinct is to protect your child, and there is nothing you can do. It is crushing. Our beautiful son had big dreams, an indomitable spirit, and was ready to continue fighting, and we had no tools to give him. How do you explain to a seven-year-old that the doctors don’t know what to do? We researched exhaustively and we couldn’t find any children who survived medulloblastoma if a relapse occurred after a child received radiation therapy. Preventing relapse is key to children surviving. We could only find one study addressing the treatment of leptomeningeal spread of medulloblastoma, and it was preliminary in nature. There was no hope to be found.”, says Anne.
[ Keith, age 4 ] Darcee and Brent Burnett’s son, Keith, was a child affected by medulloblastoma. Darcee comments, “Our experience with metastatic medulloblastoma was devastating. We literally watched our son, Keith deteriorate before our eyes. The treatment options were grim considering we had no guarantee they would work and even if they did, there were serious lifelong side-effects. Once the initial treatment didn’t work, we had no options. There was no plan available for treatment. That is something no parent should ever hear.It was important to us that after he passed, Keith’s tumor tissue was donated to research in hopes of finding better treatment options. We miss him more than can be imagined and in his memory, it is our goal to continue to fund research like this to help other children and families from heartache and loss. We are grateful and extremely hopeful by these research findings.” Anne and Kent White had a similar experience for their affected son, Zach. “My son Zach was diagnosed with medulloblastoma at the age of 4. He endured fifteen months of surgery, chemotherapy and radiation, yet the cancer returned. At that time, there was no hope of survival. The doctors did not have any proven treatments to deal with Zach’s cancer once it metastasized. As a parent it is devastating to look at your beautiful, vibrant child and know their fate is sealed because of a 3 mm. spot on their brain. As a parent your instinct is to protect your child, and there is nothing you can do. It is crushing. Our beautiful son had big dreams, an indomitable spirit, and was ready to continue fighting, and we had no tools to give him. How do you explain to a seven-year-old that the doctors don’t know what to do? We researched exhaustively and we couldn’t find any children who survived medulloblastoma if a relapse occurred after a child received radiation therapy. Preventing relapse is key to children surviving. We could only find one study addressing the treatment of leptomeningeal spread of medulloblastoma, and it was preliminary in nature. There was no hope to be found.”, says Anne.  [ Zach (right), age 5, with his family ] Zach’s mother adds, “We are so grateful for the work done by cc-TDI. Their team is committed to improving survival rates for some of the most difficult to treat childhood cancers. Through collaboration and innovative thinking, they will bring safe treatments to children as quickly as possible. The young children fighting intractable cancers don’t have years to wait for several permutations of clinical trials to play out. They need a cure and they need it now. This study provides real hope. Hopefully doctors will be able use these new findings soon to treat their patients with drugs that have already been approved by the FDA.” Collaborators on the study included Drs. Yoon-Jae Cho (Stanford University), Darrell Bigner (Duke University), Atiya Mansoor and Randall Woltjer (Oregon Health & Science University) and Joel Michalek (University of Texas Health Science Center). Funding was provided in part by the Rally Foundation, whose director Dean Crowe remarked, “We at Rally see ourselves as philanthropic seed investors, providing funding for the next great discovery in childhood cancer research. We are proud of the progress that this important medulloblastoma research is making. The potential to avoid radiation and its horrific side effects by repurposing shelved drugs to stop the spread of medulloblastoma provides great hope for children and their families fighting this beast. This collaborative research aligns with our mission to discover better treatments and ultimately, cures.” For more information on cc-TDI’s mission to move scientific discoveries to clinical trials for children with cancers like medulloblastoma, visit www.cc-TDI.org. [ funding acknowledgements: These studies were supported in part by a pilot grant fund from the National Cancer Institute (2P30CA069533), a gift from Matthew Nelson and the Wesley’s Cure for Cancer Research Foundation (WCCRF) for medulloblastoma research, funds by the Schnitzer Investment Corporation and programmatic support of the Rally Foundation. Key equipment was made possible by gifts from the Kyla McCullough Gift Fund. We thank Nancy Goodman, whose critical questions inspired these studies. ] ### About Children’s Cancer Therapy Development Institute The Children’s Cancer Therapy Development Institute (cc-TDI, www.cc-tdi.org) is a unique non-profit organization focused on the ‘preclinical gap’ in childhood cancer research. Our mission is to bridge scientific discovery and the initiation of clinical trials. Through our efforts, we will provide evidence-based testing for the selection of new drugs to be used in childhood cancer clinical trials, thus seeding pediatric Phase I and II trials. This concept was emphasized in the Institute of Medicine Report, Making Better Drugs for Children with Cancer in 2005. Our longstanding work with mouse models of brain tumors and sarcomas is the cornerstone for basic science & target discovery, as well as preclinical studies, for our mission. The cc-TDI research team is led by Scientific Director Dr. Charles Keller who follows in the footsteps of his mentor, 2007 Nobel laureate Mario Capecchi. The cc-TDI laboratory is based on the premise of a non-profit multidisciplinary biotech and is thus located in between the Silicon Forest in Hillsboro OR (Intel headquarters) and the Portland-area medical center. Our 4600 sq ft BSL2 wet lab facility is a former 70-year old paint factory remodeled by Nike as an off-site creative space – an ideal setting to spark innovation. Contacts: Charles Keller, MD(801) 232-8038 | charles@cc-TDI.orgJonathan Agin | (703) 371-0218 jonathan@cc-tdi.org
[ Zach (right), age 5, with his family ] Zach’s mother adds, “We are so grateful for the work done by cc-TDI. Their team is committed to improving survival rates for some of the most difficult to treat childhood cancers. Through collaboration and innovative thinking, they will bring safe treatments to children as quickly as possible. The young children fighting intractable cancers don’t have years to wait for several permutations of clinical trials to play out. They need a cure and they need it now. This study provides real hope. Hopefully doctors will be able use these new findings soon to treat their patients with drugs that have already been approved by the FDA.” Collaborators on the study included Drs. Yoon-Jae Cho (Stanford University), Darrell Bigner (Duke University), Atiya Mansoor and Randall Woltjer (Oregon Health & Science University) and Joel Michalek (University of Texas Health Science Center). Funding was provided in part by the Rally Foundation, whose director Dean Crowe remarked, “We at Rally see ourselves as philanthropic seed investors, providing funding for the next great discovery in childhood cancer research. We are proud of the progress that this important medulloblastoma research is making. The potential to avoid radiation and its horrific side effects by repurposing shelved drugs to stop the spread of medulloblastoma provides great hope for children and their families fighting this beast. This collaborative research aligns with our mission to discover better treatments and ultimately, cures.” For more information on cc-TDI’s mission to move scientific discoveries to clinical trials for children with cancers like medulloblastoma, visit www.cc-TDI.org. [ funding acknowledgements: These studies were supported in part by a pilot grant fund from the National Cancer Institute (2P30CA069533), a gift from Matthew Nelson and the Wesley’s Cure for Cancer Research Foundation (WCCRF) for medulloblastoma research, funds by the Schnitzer Investment Corporation and programmatic support of the Rally Foundation. Key equipment was made possible by gifts from the Kyla McCullough Gift Fund. We thank Nancy Goodman, whose critical questions inspired these studies. ] ### About Children’s Cancer Therapy Development Institute The Children’s Cancer Therapy Development Institute (cc-TDI, www.cc-tdi.org) is a unique non-profit organization focused on the ‘preclinical gap’ in childhood cancer research. Our mission is to bridge scientific discovery and the initiation of clinical trials. Through our efforts, we will provide evidence-based testing for the selection of new drugs to be used in childhood cancer clinical trials, thus seeding pediatric Phase I and II trials. This concept was emphasized in the Institute of Medicine Report, Making Better Drugs for Children with Cancer in 2005. Our longstanding work with mouse models of brain tumors and sarcomas is the cornerstone for basic science & target discovery, as well as preclinical studies, for our mission. The cc-TDI research team is led by Scientific Director Dr. Charles Keller who follows in the footsteps of his mentor, 2007 Nobel laureate Mario Capecchi. The cc-TDI laboratory is based on the premise of a non-profit multidisciplinary biotech and is thus located in between the Silicon Forest in Hillsboro OR (Intel headquarters) and the Portland-area medical center. Our 4600 sq ft BSL2 wet lab facility is a former 70-year old paint factory remodeled by Nike as an off-site creative space – an ideal setting to spark innovation. Contacts: Charles Keller, MD(801) 232-8038 | charles@cc-TDI.orgJonathan Agin | (703) 371-0218 jonathan@cc-tdi.org






